Hip Osteoarthritis – Causes, Symptoms, Diagnosis & Treatment
Hip osteoarthritis is a condition in which the smooth cartilage covering the ball-and-socket hip joint gradually wears away. As the cartilage becomes thinner, the bones start rubbing against each other, leading to pain, stiffness and reduced movement.
It is one of the most common causes of chronic hip pain in adults.
Early treatment and lifestyle modifications can significantly slow the progression and improve quality of life.
Why Does Hip Osteoarthritis Occur?
Hip arthritis develops slowly over many years. Common reasons include:
1. Age-related wear and tear
The cartilage naturally becomes thinner as we get older.
2. Previous injury
Hip fractures, childhood hip disorders or earlier trauma may lead to arthritis later.
3. Genetics
Some people inherit a tendency for early cartilage degeneration.
4. Obesity
Extra weight increases the load on the hip joint.
5. Abnormal hip structure
Conditions like developmental dysplasia, Perthes disease or femoroacetabular impingement (FAI) can lead to early arthritis.
6. Inflammatory conditions
Rheumatoid arthritis, gout or infections may damage joint cartilage.
Common Symptoms of Hip Osteoarthritis
Patients often experience:
- Pain in the groin, thigh or buttock
- Stiffness, especially after sitting or resting
- Difficulty walking long distances
- Pain while climbing stairs or standing from a chair
- Reduced ability to rotate or bend the hip
- A feeling of the joint “catching” or “locking”
- Limping (in later stages)
Symptoms usually worsen gradually but can flare up with activity.
Diagnosis
Diagnosis includes:
1. Clinical evaluation
- Nature and location of pain
- Range of movement
- Gait (walking pattern)
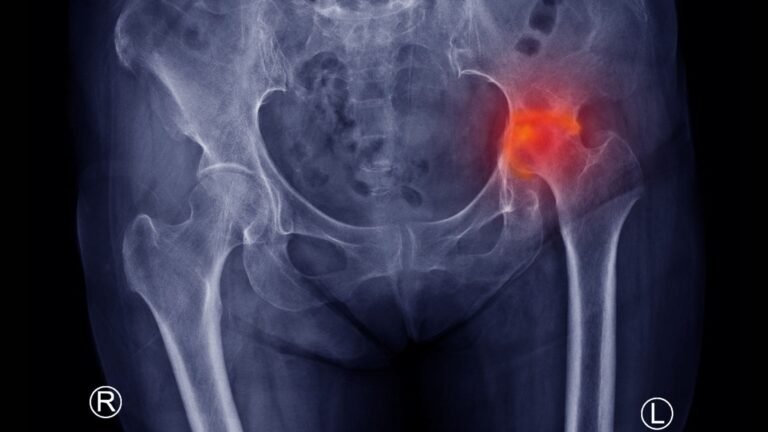
2. X-ray
The most important test for hip osteoarthritis. It shows:
- Narrowed joint space
- Bone spurs (osteophytes)
- Bone hardening beneath cartilage (sclerosis)
3. MRI (if needed)
Used in early cases or when soft tissue problems are suspected.
Treatment Options
Treatment depends on severity. Many patients improve without surgery in the early stages.
1. Non-Surgical Management
Medications
- Pain relievers
- Anti-inflammatory drugs (as advised by doctor)
Physiotherapy
- Hip mobility exercises
- Strengthening of core, gluteal and thigh muscles
- Gait training
- Posture and lifestyle guidance
Activity Modification
- Avoid prolonged sitting, squatting or cross-leg sitting
- Use supportive footwear
- Switch to low-impact exercises such as walking, cycling or swimming
Weight Management
Reduces pressure on the hip and helps slow joint damage.
Injections
In selected cases:
- Steroid injection for inflammation
- Viscosupplementation (hyaluronic acid) for lubrication
- PRP / biologics in early arthritis (depending on case)
2. Surgical Options
Surgery is considered when pain interferes with routine activities and non-surgical treatment no longer helps.
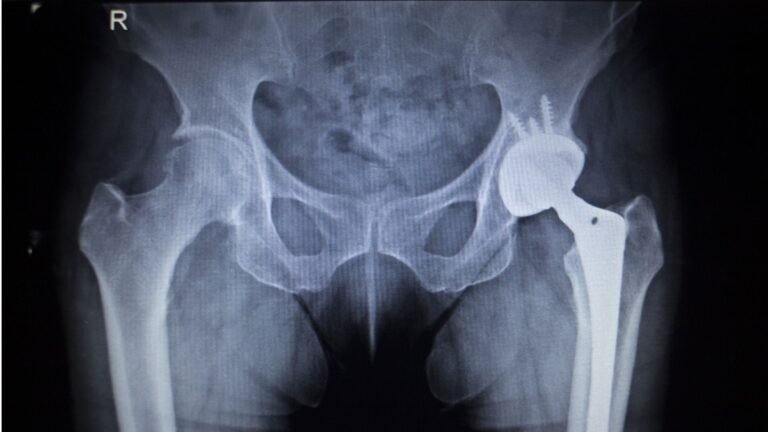
Hip Replacement (Total Hip Arthroplasty)
The damaged ball and socket are replaced with artificial components that restore smooth movement.
Benefits include:
- Major pain relief
- Improved walking
- Better range of motion
- Long-lasting function (15–20 years or more)
Minimally invasive options such as the Direct Anterior Approach provide faster recovery and fewer movement restrictions.
Self-Care Tips for Hip Arthritis
- Stay active; avoid long periods of rest
- Maintain a healthy weight
- Use heat therapy to ease stiffness
- Strengthen hip and core muscles regularly
- Avoid high-impact activities like running on hard surfaces
- Use a walking stick temporarily if needed (held in opposite hand of affected hip)
Key Takeaway
Hip osteoarthritis is a progressive but manageable condition. With early diagnosis, focused physiotherapy, lifestyle adjustments and — when necessary — surgical intervention, most patients can regain comfortable mobility and return to normal activities.