Arthroscopic PCL Repair / Reconstruction
The Posterior Cruciate Ligament (PCL) is one of the key stabilizing ligaments of the knee. When it tears due to trauma, patients may experience deep knee pain, difficulty walking downhill or downstairs, and a feeling of the knee “giving way.”
If the ligament does not heal properly, arthroscopic PCL repair or reconstruction can restore stability and protect the knee from long-term damage.
What Is Arthroscopic PCL Repair / Reconstruction?
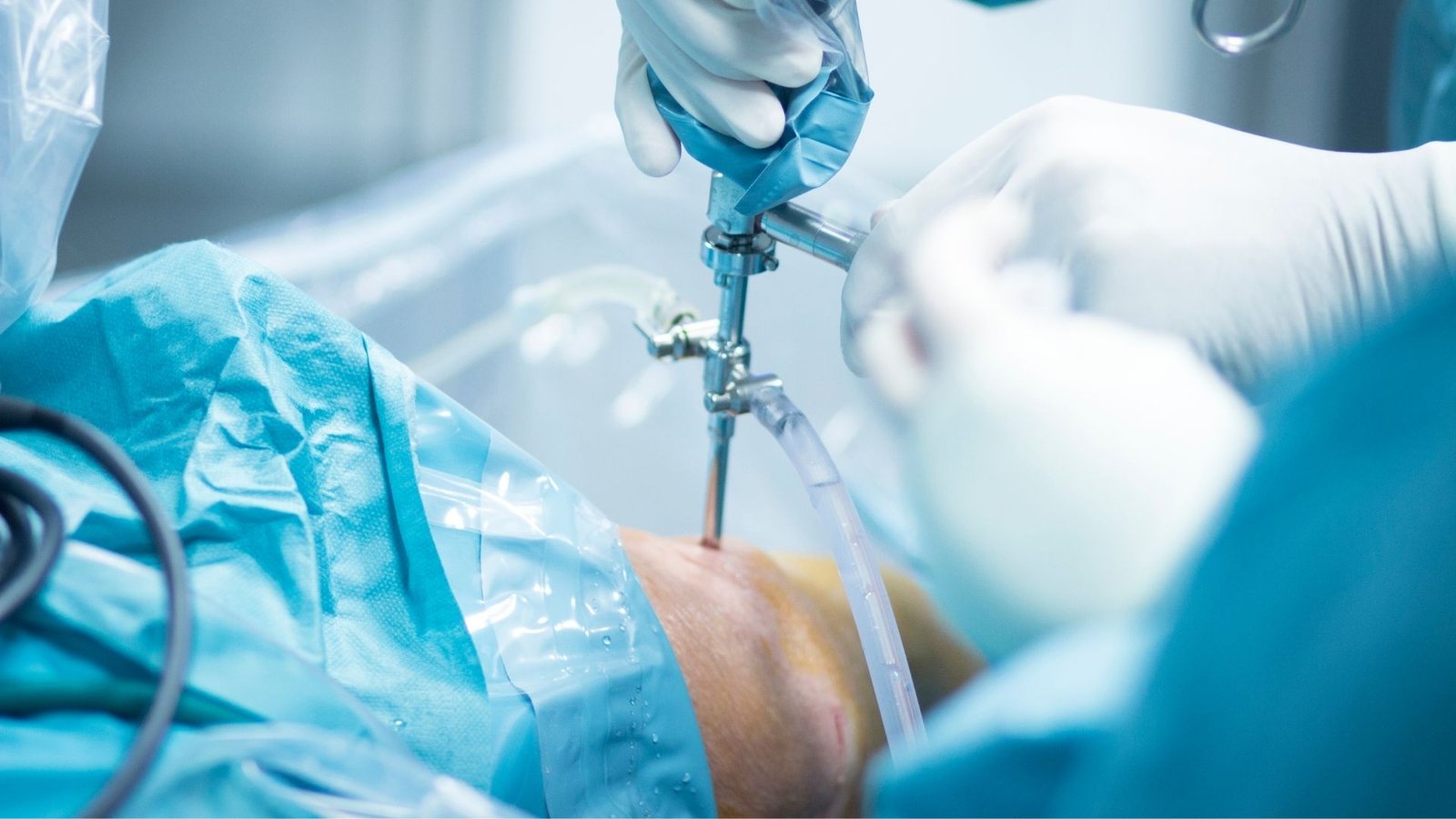
PCL surgery is performed using keyhole (arthroscopic) techniques, which means only tiny incisions are made around the knee. A high-definition camera and fine instruments are inserted to repair or reconstruct the torn ligament with precision.
Depending on the type and location of the tear
Arthroscopic PCL Repair
If the ligament has peeled off cleanly from its attachment and tissue quality is good, the surgeon may reattach it using sutures and anchors.
Arthroscopic PCL Reconstruction
More commonly, the torn PCL needs to be replaced with a graft, which acts as a new ligament. Grafts are usually taken from:
- Hamstring tendons
- Peroneus longus tendon
- Quadriceps tendon
- Allograft (donor tendon) in select cases
The graft is placed exactly where the original PCL was, restoring normal knee biomechanics.
Who Should Consider Arthroscopic PCL Surgery?
Surgery is recommended for patients who have:
- Complete PCL tears
- Instability that interferes with sports or daily activities
- Persistent symptoms despite physiotherapy
- Multiligament injuries (PCL + ACL / MCL / LCL)
- High-demand professions or athletic goals
Early surgical stabilization helps prevent meniscus damage and early arthritis.
Advantages of Arthroscopic PCL Surgery
Compared to older open procedures, the arthroscopic technique offers:
- Small incisions, minimal scarring
- Reduced blood loss and less postoperative pain
- Better visualization of the joint structures
- Preservation of normal tissues
- Faster recovery and rehabilitation
- High long-term success when done with proper rehab
The goal is not just to stop instability but to restore confidence, function and knee longevity.
How the Procedure Is Performed
A simplified overview:
- Surgery is performed under spinal or general anaesthesia.
- Two or three keyhole incisions are made around the knee.
- The torn PCL is visualized with the arthroscope.
- Depending on the injury:
- Repair – ligament reattached with sutures/anchors
- Reconstruction – graft prepared and positioned using tunnels in femur and tibia
- Fixation is secured and stability is confirmed.
- The wounds are stitched and a sterile dressing is applied.
Patients usually begin walking with support the same or next day, depending on protocol.
Recovery Timeline
Healing takes time because the PCL deep inside the knee requires gradual graft integration.
| Time After Surgery | Progress |
|---|---|
| First 6 weeks | Brace support, assisted walking, early therapy |
| 6–12 weeks | Improved mobility & strengthening |
| 3–6 months | Functional training and light jogging |
| 6–9 months | Sports-specific training |
| 9–12 months | Return to pivoting / contact sports (only after clearance) |
A structured physiotherapy program is essential for the best results.
Success & Expectations
Most patients return to:
- Walking without hesitation
- Gym and sports activities
- Daily tasks without fear of instability
High-level athletes can also return to competitive sport with proper rehabilitation.
Key Takeaway
Arthroscopic PCL repair or reconstruction is a highly effective and minimally invasive solution for PCL injuries that do not heal on their own. By restoring knee stability early, the procedure protects the joint from future wear-and-tear and helps patients regain an active, confident and pain-free life.