Avascular Necrosis (AVN) of the Hip – Causes, Symptoms, Diagnosis & Treatment
Avascular Necrosis (AVN) of the hip — also called osteonecrosis — is a condition where the blood supply to the head of the femur (ball of the hip joint) gradually reduces. Without enough blood flow, the bone becomes weak, starts to collapse, and the smooth joint surface gets damaged.
If not treated early, AVN can lead to early arthritis, severe pain and difficulty walking.
Why Does AVN Occur?
AVN develops when the blood flow to the hip bone is interrupted. Common causes include:
1. Long-term steroid use
One of the most common reasons.
2. Alcohol consumption
Heavy alcohol intake weakens bone cells and blood vessels.
3. Trauma
A hip fracture or dislocation can directly damage the blood supply.
4. Medical conditions
- Sickle cell disease
- Autoimmune disorders
- Kidney disease
- Pancreatitis
5. Unknown reasons (Idiopathic)
Many young and healthy individuals develop AVN without any identifiable cause.
AVN is most commonly seen in people between 20–50 years of age.
Symptoms of AVN of the Hip
Early AVN may not cause noticeable symptoms. As the disease progresses, patients may experience:
- Groin pain, sometimes felt in the thigh or buttock
- Pain that increases with walking or weight-bearing
- Difficulty sitting cross-legged or squatting
- Stiffness in the hip
- Limping
- Pain at night in advanced stages
If the bone collapses, the pain becomes more constant and severe.
Diagnosis
Diagnosis usually includes:
Clinical Examination
Evaluation of pain location, movement restriction and walking pattern.
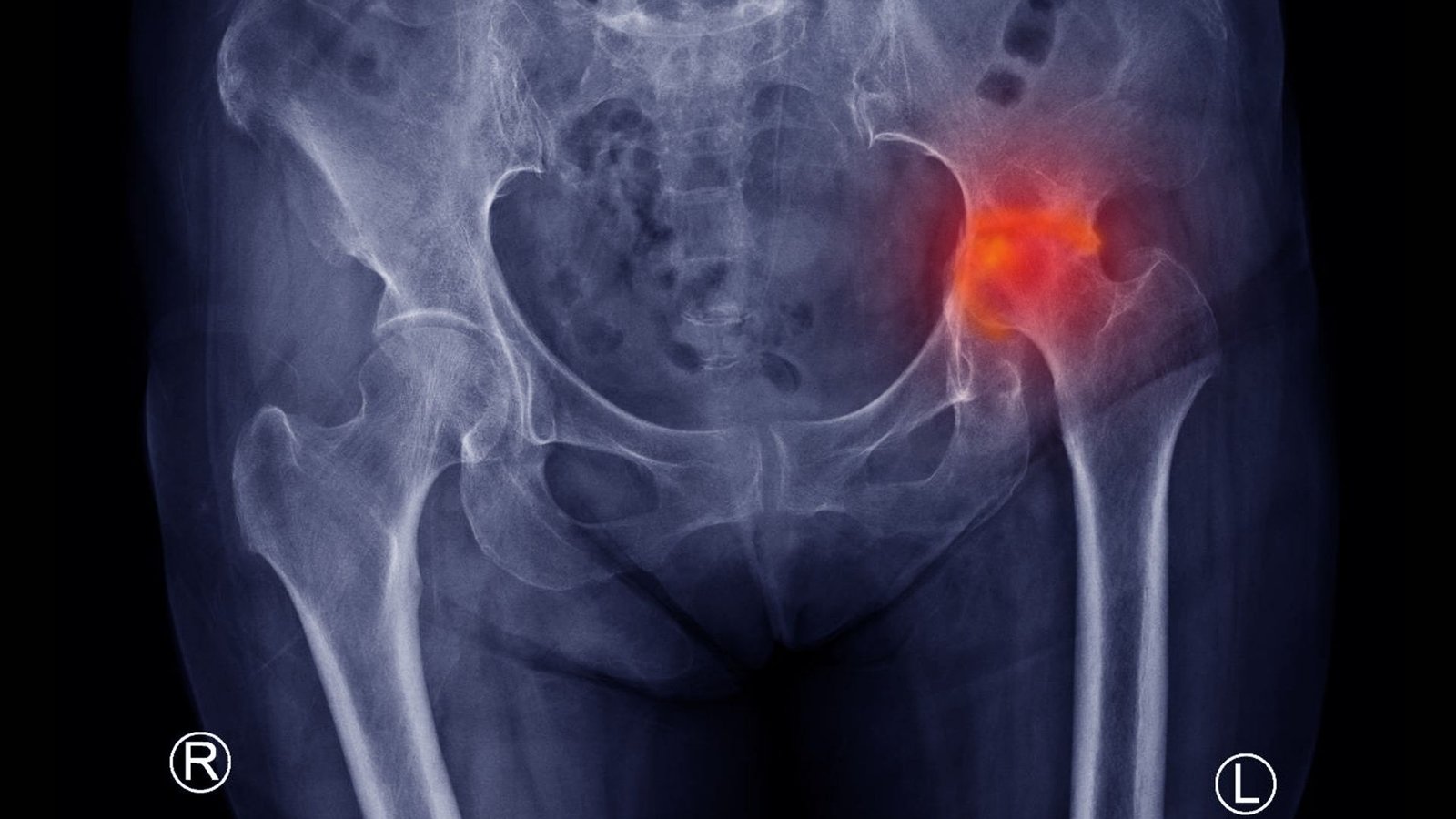
X-ray
Shows changes in bone shape and joint surface, especially in later stages.
MRI
The most sensitive test. It detects AVN very early, even before changes appear on X-ray.
Early diagnosis is important to preserve the hip joint and delay or avoid joint replacement.
Stages of AVN
AVN is classified into stages:
- Early stage – Blood supply reduced, but bone shape is maintained
- Collapse stage – Bone begins to cave in
- Advanced stage – Joint surface damaged; secondary arthritis develops
Treatment decisions depend heavily on the stage at diagnosis.
Treatment Options
1. Non-Surgical Management (Early Stages)
These methods aim to slow the disease but cannot reverse AVN:
- Medication for pain
- Reduced weight-bearing
- Physiotherapy for hip mobility
- Bisphosphonates in select cases
- PRP or stem-cell–based injections (evidence still evolving)
Non-surgical options are most effective before bone collapse.
2. Core Decompression (Early to Mid Stages)
A minimally invasive surgery where a channel is created inside the femoral head to:
- Reduce pressure
- Improve blood flow
- Relieve pain
- Slow progression of AVN
Sometimes bone grafts or biologic materials (stem cells/PRP) are added to improve healing.
This procedure is ideal when the femoral head is still intact.
3. Femoral Head–Preserving Procedures
For selected patients:
- Bone grafting
- Osteotomy (realigning the bone)
These procedures aim to save the natural hip joint and delay arthritis.
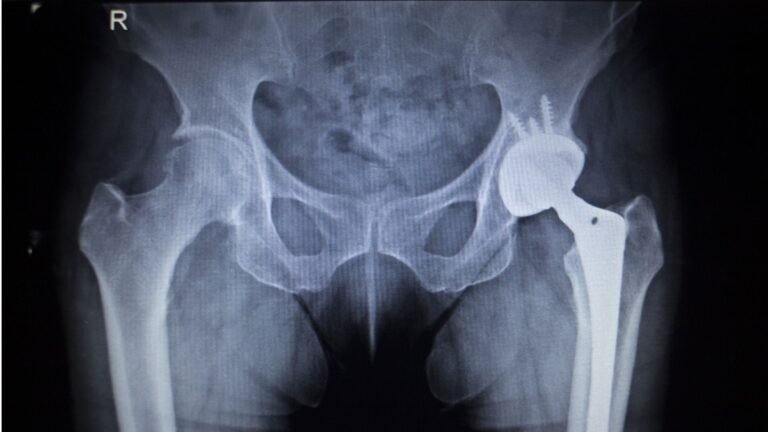
4. Total Hip Replacement (Advanced AVN)
When the femoral head collapses or arthritis has developed, hip replacement becomes the best option.
The damaged ball and socket are replaced with artificial components, giving:
- Excellent pain relief
- Smooth hip movement
- Ability to walk and perform daily activities comfortably
Modern techniques such as the Direct Anterior Approach allow faster recovery with minimal muscle damage.
Self-Care & Lifestyle Guidance
For patients diagnosed with AVN:
- Avoid high-impact activities
- Reduce or stop alcohol
- Avoid long-term steroid use unless medically necessary
- Maintain a healthy weight
- Do physiotherapy regularly to keep the hip mobile
Early lifestyle adjustments can significantly slow disease progression.
Key Takeaway
Avascular Necrosis of the hip is a progressive condition, but early diagnosis and timely treatment can preserve the hip joint and delay the need for replacement.
Advanced AVN responds very well to hip replacement surgery, offering long-term pain relief and excellent function.